How does gingivitis and periodontitis develop?
The prime cause of gingivitis and of the periodontitis that develops from it are bacteria, according to our so far undisputed state of knowledge. These are germs organised in special complexes, in so-called bacterial biofilms. Certain local conditions may lead to these biofilms spreading from the edges of the gums along the surface of the roots of the teeth. These local conditions might be, for example, badly fitting fillings or crowns, but also tartar and crooked teeth. In addition to these factors, lack of oral hygiene with insufficient removal of plaque also favours the development of this kind of biofilm on the root surfaces. The consequences are that, under the gums, with time, particularly aggressive bacteria can establish themselves which would not form in the presence of oxygen. Some of these may even penetrate the soft tissue and release certain toxins. This leads to a destruction of the soft tissue collar surrounding the tooth. Similarly, the body's immune defence against these bacteria also leads to a destruction of the tissue. The result is an inflammation of the gums which leads to the periodontal tissue no longer fitting tightly to the tooth. A case of gingivitis has developed with a pathological periodontal pocket.
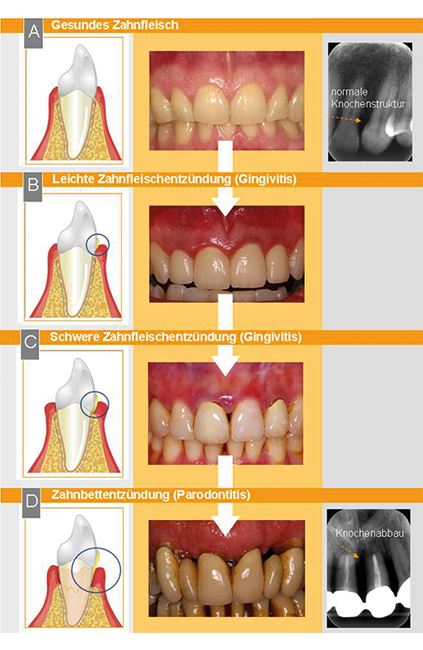
To the extent that the body's own immune defence can hold the tissue-destroying bacteria in check, without treatment the inflammation will remain limited to the gums for quite some time. But this may change as soon as certain systemic conditions impair the immune defence, for example stress, or genetic factors. i.e. a hereditary predisposition, but also general diseases like diabetes mellitus. Furthermore, one of the major influencing factors is smoking. This leads to the inflammation advancing beyond the gums. Both the bacteria and the inflammatory substances from the body's own immune defence system can then cause deterioration of the fibre structure that surrounds the root and supports the tooth, and of the surrounding bone. A case of periodontitis has developed.